Sciatica can feel like more than “back pain.” It is often a sharp, electric, or burning pain that starts in the low back or buttock and travels down the leg, sometimes with numbness, tingling, or weakness. When it flares, most people are not looking for theory, they want relief that actually lasts.
A sciatica chiropractor can be one part of an evidence-informed plan, especially when care is targeted at the underlying driver (for example, nerve irritation from the low back, hip mechanics, muscle tension, or movement habits). Below are the relief options that tend to work best, what they do, and how to choose the right approach for your symptoms.
What sciatica is (and what it is not)
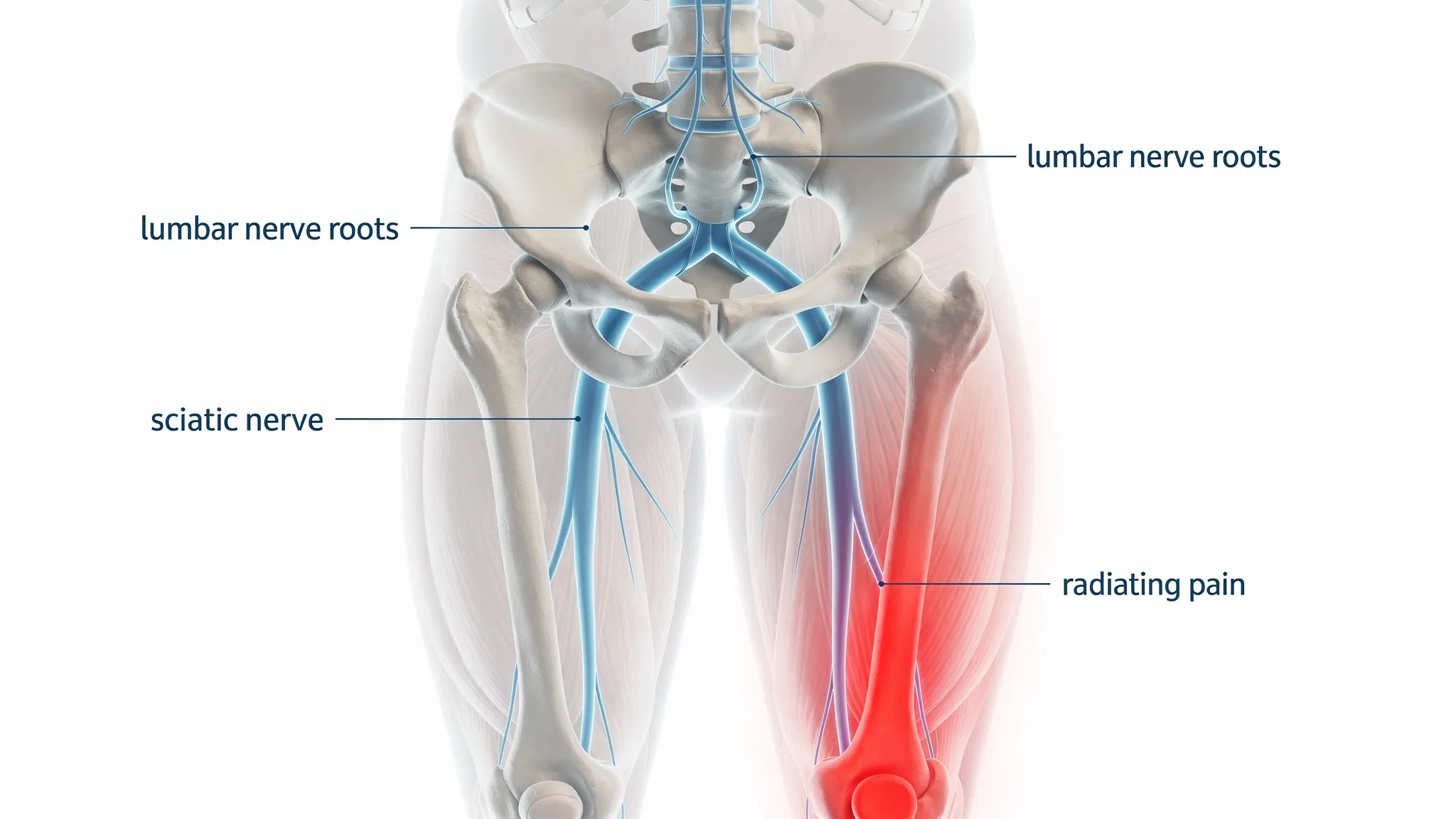
“Sciatica” describes symptoms from irritation or compression of the sciatic nerve or its nerve roots, most commonly in the lumbar spine. It is not a diagnosis by itself. Common causes include:
- Lumbar disc herniation irritating a nerve root
- Spinal stenosis (narrowing around nerves), often worse with walking or standing
- Piriformis or deep gluteal syndrome (nerve irritation in the buttock region)
- Joint and movement contributors (hip stiffness, pelvic mechanics, poor tolerance to sitting)
Many cases improve with conservative care. Major guidelines for low back pain emphasize starting with non-drug, non-surgical options when serious causes are not suspected, and escalating only when needed. For example, the American College of Physicians recommends nonpharmacologic treatments (such as exercise-based therapy, spinal manipulation, acupuncture) as first-line options for many types of back pain presentations, depending on duration and context (ACP guideline). Sciatica is more specific than generic low back pain, but it commonly follows the same stepwise logic: rule out red flags, calm the pain, restore motion and strength, then prevent recurrence.
When sciatica is an emergency (do not “wait and see”)
Sciatica-like pain is usually not dangerous, but certain symptoms need urgent medical evaluation.
| Red flag symptom | Why it matters | What to do now |
|---|---|---|
| New loss of bowel or bladder control | Possible cauda equina syndrome | Go to the ER immediately |
| Saddle anesthesia (numbness in groin/perineum) | Possible cauda equina syndrome | Go to the ER immediately |
| Progressive leg weakness (foot drop, worsening strength loss) | Nerve compromise | Same-day urgent evaluation |
| Fever, unexplained weight loss, cancer history, IV drug use | Infection or malignancy risk | Urgent medical evaluation |
| Major trauma, osteoporosis with sudden severe pain | Fracture risk | Urgent imaging/assessment |
If you are unsure, err on the side of getting checked out.
What a sciatica chiropractor can actually help with
Effective chiropractic care for sciatica is less about “cracking a back” and more about a structured clinical process:
- Confirm whether symptoms behave like nerve pain (radiation pattern, tingling, neuro tests)
- Identify the driver (disc-related pattern, stenosis pattern, hip/piriformis pattern, movement sensitivity)
- Choose the right tools for that driver (manual care, graded movement, rehab, activity modifications)
- Track objective changes (pain distribution, walking tolerance, strength, straight-leg raise tolerance)
When people search “sciatica chiropractor near me,” the most important filter is not distance, it is whether the clinic can evaluate nerve-related symptoms carefully and combine hands-on care with a rehab plan that sticks.
Relief options that work (and how to choose among them)
Sciatica relief typically comes from combining a few complementary options rather than relying on a single technique.
1) Movement-based relief (often the fastest “self-care” win)
For many cases, the most effective early strategy is finding the positions and movements that centralize symptoms (pain moves out of the leg and back toward the low back) or at least reduce intensity.
Common examples:
- Short walking bouts throughout the day, if walking reduces symptoms
- Gentle repeated movements that reduce leg symptoms (some people respond to extension-based patterns, others do not)
- Avoiding prolonged sitting early on, using timed breaks
Why it works: nerve irritation is often sensitive to load and posture. Small, frequent movement “doses” can calm the system and restore tolerance.
A clinician (chiropractor, physical therapist, sports medicine provider) can help you determine the safest direction to bias and what to avoid.
2) Spinal manipulation or mobilization (targeted, not one-size-fits-all)
Spinal manipulation is included in major clinical guidelines for certain back pain scenarios (ACP guideline). For sciatica, the evidence base is more mixed and highly dependent on proper patient selection, but many patients report meaningful improvement when manipulation is applied appropriately and paired with exercise.
What it may help with:
- Pain modulation (reducing perceived pain)
- Restoring segmental motion
- Reducing protective muscle guarding
When it is less likely to help: severe, progressive neurological deficits, or when pain is driven primarily by non-mechanical causes.
A good plan should include reassessment. If leg symptoms worsen or do not change after a reasonable trial, the strategy should be adjusted.
3) Soft tissue work and nerve “gliding” strategies
Not all radiating leg pain is purely spine-driven. Irritated tissues around the hip, deep gluteal area, hamstrings, or calf can amplify symptoms.
Options that often help:
- Soft tissue therapy for gluteal and hip rotators
- Mobility work for hip flexors and hamstrings, when appropriate
- Neural mobilization (nerve glides) used carefully (too aggressive can flare symptoms)
A practical sign you are on the right track: symptoms become less sharp, travel less far down the leg, and you can tolerate sitting or walking longer.
4) Acupuncture for pain relief and muscle tone regulation
Acupuncture is also recommended as a nonpharmacologic option in guidelines for chronic low back pain in appropriate patients (ACP guideline). While sciatica-specific results vary by study, acupuncture can be useful when pain is limiting sleep, movement, or rehab participation.
In integrated care, acupuncture is commonly used to:
- Reduce pain sensitivity
- Address muscle tension that perpetuates guarding
- Improve comfort enough to progress rehab
5) Physical therapy style rehabilitation (the “stay better” phase)
Even when pain calms down, recurrence is common if strength, mobility, and daily mechanics are not addressed. Rehab focuses on restoring capacity.
A sciatica-focused program often includes:
- Hip and trunk strength (glutes, deep core, anti-rotation control)
- Gradual return to loaded patterns (hinge, squat variations, carries)
- Workstation and lifting coaching
- Graded exposure back to sitting, running, or sport
The best programs are individualized and progressed based on function, not just pain.
6) Pain management options when conservative care stalls
If pain remains severe, function is not improving, or symptoms suggest a more complex pain generator, a broader pain management plan can be appropriate.
Depending on the clinical scenario and scope of practice, this may include coordinated care such as:
- Trigger point injections for severe muscle spasm contributors
- Referral for imaging when indicated
- Co-management with a physician for medication strategy when truly necessary
The goal is not “more interventions,” it is the minimum effective escalation that restores function.
A quick “pattern guide” to match symptoms with likely drivers
This table is not a diagnosis, but it can help you understand why one sciatica plan works for your friend and not for you.
| Symptom pattern | Common clue | Often responds to |
|---|---|---|
| Worse with sitting, bending forward, coughing/sneezing | Disc-related irritation is more likely | Activity modification, directional movements, manual care plus rehab |
| Worse with walking/standing, better sitting or bending slightly forward | Stenosis-like pattern is more likely | Flexion-tolerant exercises, pacing, hip mobility, strengthening |
| Buttock-dominant pain with limited hip rotation, provoked by prolonged sitting | Deep gluteal/piriformis contributors | Soft tissue work, hip mobility, graded loading |
| Tingling/numbness with clear weakness | Higher nerve involvement | Prompt evaluation, careful progression, possible imaging/referral |
If you have progressive weakness or major numbness, do not self-triage.
What to expect at a chiropractic visit for sciatica
A sciatica-focused evaluation should look more like a clinical exam than a quick massage.
History that matters
Expect questions about:
- Where the pain travels (back only, buttock, below the knee)
- Numbness, tingling, or weakness
- What makes it worse or better (sitting, walking, bending)
- Sleep disruption and work limitations
- Prior episodes and what helped
Physical exam that matters
Common components include:
- Neurological screening (reflexes, strength, sensation)
- Range of motion and movement tolerance testing
- Provocation tests (for example, straight-leg raise variants)
- Hip screening
Imaging (only when it changes management)
Many cases do not need immediate imaging. Clinical guidance often recommends reserving imaging for red flags or when results would change the plan (for example, persistent deficits, severe symptoms not improving). A helpful patient-friendly overview is available from the American Academy of Family Physicians.
How long does it take to feel better?
Timelines vary, but two principles are consistent:
- Early wins often come from reducing sensitivity, improving sleep, and finding tolerable movement.
- Long-term wins come from rebuilding capacity so the nerve and surrounding tissues are not repeatedly irritated.
Many acute sciatica episodes improve over weeks, especially when activity is modified and progressive rehab is started early. If pain is unchanged, worsening, or disabling after a reasonable trial of conservative care, reassessment and escalation may be appropriate.
How to choose a sciatica chiropractor (without guessing)
Look for signs of a structured approach:
- They screen for red flags and neurological deficits
- They explain the most likely pain driver in plain language
- They give you a home plan on day one (not just passive care)
- They track progress with functional measures (walking tolerance, sitting time, strength)
- They can integrate or coordinate other services when needed (rehab, acupuncture, pain management)
Avoid clinics that promise to “fix any sciatica” in a preset number of visits. Sciatica is a symptom pattern with multiple causes, and honest care reflects that.
Integrated care in New York: why combining approaches can be a game changer
Sciatica is often multi-factorial: joint mechanics, irritated nerve tissue, muscle guarding, and stress-related pain sensitivity can all coexist. That is why integrated care can work well in practice.
At Move Well MD in Manhattan, care is centered on helping patients move freely with a combination of chiropractic care, acupuncture treatments, pain management, and physical rehabilitation (as clinically appropriate). If you want a plan that addresses both symptom relief and the mechanics that caused the flare in the first place, you can learn more about the clinic at Move Well MD.
The bottom line
Relief that works is rarely a single technique. The most reliable sciatica plans combine accurate assessment, targeted hands-on care (when appropriate), a clear movement strategy, and progressive rehab that restores confidence in sitting, walking, and lifting.
If your symptoms are severe, involve weakness, or are not improving, do not keep guessing. Get evaluated, make sure red flags are ruled out, and insist on a plan with measurable checkpoints.