Neck and back pain rarely comes from one single “thing.” For many New Yorkers, it’s a mix of desk posture, long commutes, stress-related muscle tension, and sudden flare-ups from lifting, training, or sleeping in a bad position. Chiro therapy can help by improving joint motion, calming irritated tissues, and rebuilding the movement patterns that keep pain coming back.
This guide breaks down the most common chiro therapy techniques used for neck and back pain, what each one is designed to do, what it typically feels like, and how clinicians decide which approach is appropriate.
What chiro therapy is (and what it is not)
Chiro therapy is a hands-on, musculoskeletal approach focused on how the spine and related joints, muscles, and nerves influence pain and movement. In practical terms, treatment often includes some combination of:
- Joint-based care (manipulation or mobilization)
- Soft-tissue work for muscles and fascia
- Rehab exercises to improve strength, control, and posture
- Education on ergonomics, lifting mechanics, sleep positioning, and recovery
It is not a replacement for emergency care, and it is not meant to “treat everything.” The best outcomes usually happen when care targets mechanical pain (pain tied to movement, posture, or tissue irritation) and when treatment is paired with a plan to restore function.
Neck and back pain: the most common mechanical drivers
When someone says “my neck hurts” or “my low back is killing me,” the underlying cause is often a combination of overlapping factors rather than a single diagnosis.
Common mechanical contributors include:
- Joint stiffness or irritation (facet joints and surrounding tissues)
- Muscle strain and trigger points (often in the upper traps, levator scapulae, glutes, or hip flexors)
- Disc-related irritation (which may or may not include arm/leg symptoms)
- Movement coordination problems (poor core or scapular control, hip stiffness, forward-head posture)
- Sensitivity of the nervous system after repeated flare-ups (pain becomes easier to trigger)
A key goal of chiro therapy is to reduce pain enough to allow normal motion again, then reinforce that progress with mobility, strength, and habit changes.
When to get checked urgently (red flags)
Most neck and back pain is not dangerous, but certain symptoms deserve prompt medical evaluation. Seek urgent care if you have:
- New bowel or bladder control issues
- Progressive weakness, severe numbness, or trouble walking
- Fever, unexplained weight loss, history of cancer, or night pain that doesn’t change with position
- Recent significant trauma (fall, car crash), especially with osteoporosis risk
- Signs of possible spinal cord involvement (clumsiness, balance changes, widespread tingling)
A qualified clinician should screen for these during an initial visit and refer you out when appropriate.
How chiropractors choose the right technique
Technique selection is not supposed to be random. A solid chiro therapy evaluation typically includes:
- History (where it hurts, what triggers it, what relieves it, prior injuries)
- Range-of-motion assessment and posture/movement screens
- Neurological checks (strength, sensation, reflexes) when indicated
- Orthopedic tests for nerve tension or joint provocation
- Imaging only when clinically justified (for example, red flags, trauma, worsening neuro signs)
From there, the treatment approach is tailored based on:
- Location (neck, mid-back, low back, SI joint)
- Irritability (acute spasm versus chronic stiffness)
- Presence of nerve symptoms (radiating pain, tingling, weakness)
- Patient preference and comfort
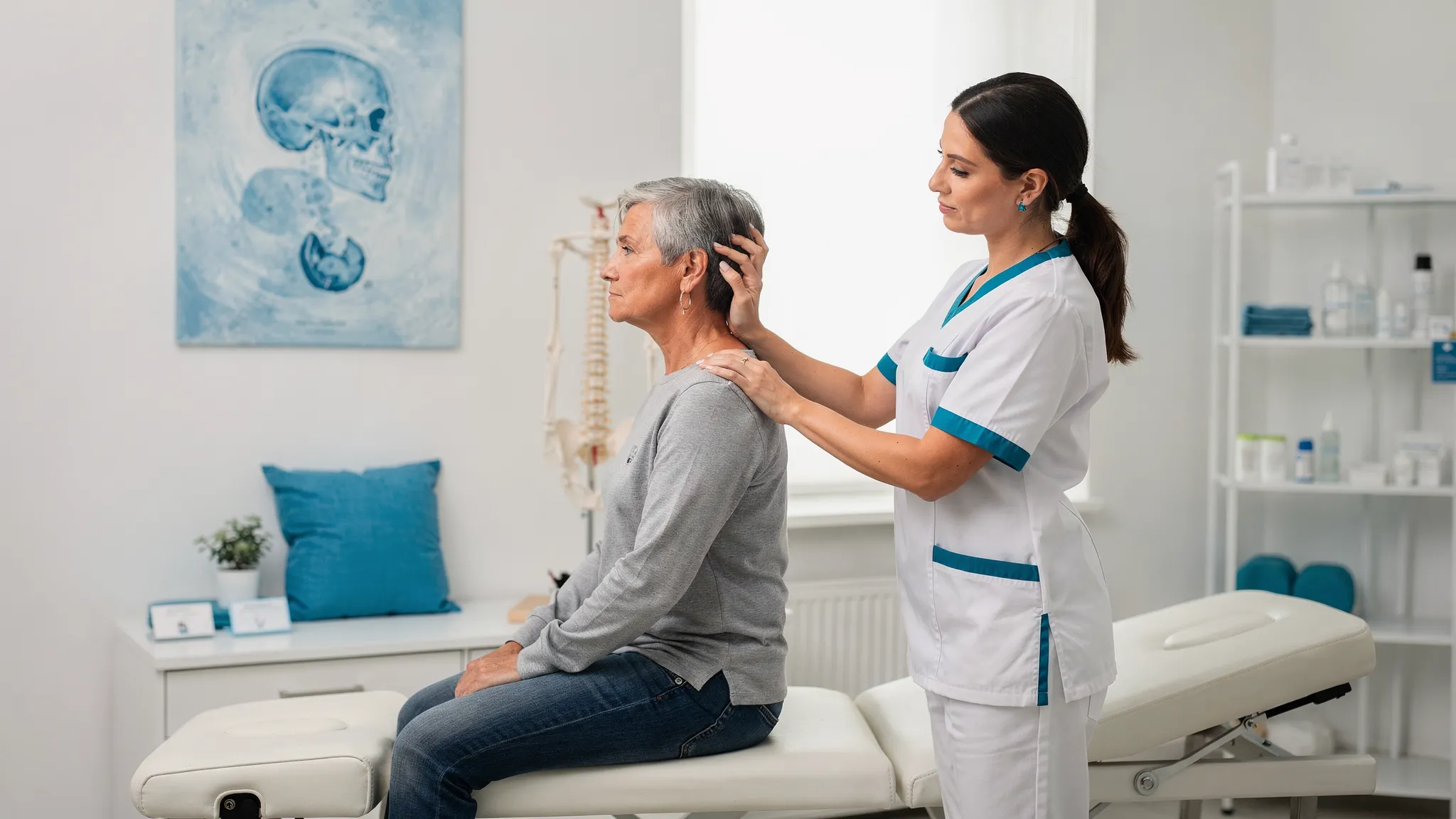
Chiro therapy techniques for neck and back pain, explained
Below are the most common techniques you may encounter in a neck or back pain plan.
1) Spinal manipulation (HVLA adjustment)
High-velocity, low-amplitude (HVLA) manipulation is the classic “adjustment.” It’s a quick, precise movement applied to a specific spinal segment.
What it’s for:
HVLA is often used to improve joint motion, reduce pain, and decrease protective muscle guarding when a segment is restricted.
What it feels like:
Typically a brief setup with a quick impulse. Some people hear a popping sound (cavitation), similar to cracking knuckles. That sound is not required for the technique to be effective.
When it may not be the best fit:
If pain is extremely irritable, if you have certain bone-health conditions, or if the clinician suspects instability, they may choose gentler options instead.
2) Spinal mobilization (gentler joint work)
Mobilization uses slower, lower-force movements through a joint’s available range.
What it’s for:
- People who prefer a less forceful approach
- Highly sensitive flare-ups
- Stiffness-dominant presentations
- Certain post-injury states where graded motion is the goal
What it feels like:
Rhythmic pressure or oscillation, often described as soothing.
3) Flexion-distraction (often used for low back pain and leg symptoms)
Flexion-distraction is performed on a specialized table that allows controlled movement (flexion and gentle traction) of the lumbar spine.
What it’s for:
This technique is commonly used when low back pain is accompanied by symptoms that may suggest disc or nerve-root irritation (for example, some cases of sciatica), or when extension-based positions feel worse.
What it feels like:
A slow, repetitive, stretching-like motion. Many patients describe it as decompressive.
4) Instrument-assisted adjustments (for example, Activator-style)
Instrument-assisted techniques use a handheld tool to deliver a small, quick impulse.
What it’s for:
- People who want to avoid manual twisting
- Older adults or those needing lower-force care
- Certain areas where a clinician wants very targeted input
What it feels like:
A light tap or click.
5) Drop-table techniques (often associated with Thompson-style)
A drop table has sections that slightly “drop” under the clinician’s thrust, reducing the amount of force needed.
What it’s for:
Commonly used for the low back, pelvis, and mid-back, especially when a lower-force adjustment is preferred.
What it feels like:
A quick thrust plus the sensation of the table section dropping a small amount.
6) Gonstead-style assessment and adjustment
Gonstead is known for a detailed biomechanical analysis (often including posture, palpation, and sometimes X-ray analysis when clinically appropriate) and specific adjustments.
What it’s for:
Precision-focused care aimed at targeted spinal segments, often used when the clinician suspects a small number of key restrictions.
What it feels like:
Typically a specific, controlled adjustment with careful setup.
7) Soft-tissue therapy (myofascial release, trigger point work)
Not all pain is joint-driven. Muscle and fascial tissues can generate significant neck and back symptoms.
What it’s for:
- Tightness and trigger points that refer pain (for example, upper trap referral into the head)
- Postural overload (desk work, carrying bags)
- Recovery support when returning to training
What it feels like:
Sustained pressure, stretching, or targeted work on tender points. Mild soreness afterward is common.
8) Rehab exercises and movement retraining (the “keep it gone” phase)
For recurring neck and back pain, exercises are often the long-term differentiator. Chiro therapy is frequently most effective when it transitions from symptom relief to function.
Common priorities include:
- Deep neck flexor and scapular control for neck pain
- Thoracic mobility work for upper-back stiffness
- Core endurance (not just max strength) for low back stability
- Hip mobility and glute strength to reduce lumbar overload
- Graded exposure back to lifting, running, or sport
If you’ve ever felt better after treatment but worse again two days later, the missing piece is often the rehab plan.
Technique comparison: what it targets and how it’s usually used
| Technique | Main goal | Typical feel | Often used when |
|---|---|---|---|
| HVLA manipulation | Restore motion, reduce pain, decrease guarding | Quick impulse, sometimes a pop | Stiff, mechanical neck/back pain without major red flags |
| Mobilization | Calm pain, gently improve motion | Slow oscillation | Acute sensitivity, preference for gentler care |
| Flexion-distraction | Reduce lumbar irritation, improve tolerance to motion | Gentle traction-like movement | Some low back pain patterns, sometimes with leg symptoms |
| Instrument-assisted | Targeted input with low force | Light tap/click | Patients who want low-force adjustments |
| Drop-table | Effective adjustment with reduced force | Quick thrust plus table drop | Pelvic/low back and mid-back issues |
| Soft-tissue therapy | Reduce muscle-driven pain and tension | Pressure and stretching | Trigger points, postural pain, overuse |
| Rehab exercise | Build resilience and prevent recurrence | Active work | Recurring pain, return to activity, posture and strength deficits |
What the research says (realistic expectations)
Clinical guidelines and reviews generally support spinal manipulation as a reasonable non-drug option for certain types of back pain.
For example, the American College of Physicians (ACP) guideline for acute and subacute low back pain recommends initial nonpharmacologic options such as spinal manipulation, heat, massage, acupuncture, and exercise-based approaches before medication in many cases (ACP guideline in Annals of Internal Medicine).
A large systematic review and meta-analysis in JAMA also found spinal manipulative therapy was associated with improvements in pain and function for acute low back pain, with effects that were modest on average but meaningful for many patients (Paige et al., JAMA 2017).
For neck pain, evidence suggests manual therapy can help certain patients, particularly when combined with exercise and education. The “best” approach often depends on whether symptoms are stiffness-dominant, movement-sensitive, or associated with headache patterns.
Bottom line: chiro therapy can be helpful, especially for mechanical neck and back pain, and tends to work best as part of a broader plan that includes movement and lifestyle changes.
Safety and side effects: what’s normal, what’s not
Most people experience either immediate relief or mild post-treatment soreness (similar to a workout) for 24 to 48 hours.
Potential short-term effects can include:
- Local soreness or stiffness
- Temporary headache (more common with upper-neck issues)
- Fatigue after a session (especially if treatment reduces long-held muscle tension)
Serious complications are uncommon, but risk depends on the technique, the region treated, and the individual’s health profile. A responsible clinician will:
- Screen for contraindications (fracture risk, infection, instability, certain vascular risks)
- Discuss options (mobilization, soft-tissue work, exercise) if higher-force techniques are not appropriate
- Encourage medical evaluation when symptoms do not fit a typical mechanical pattern
If you’re unsure whether your symptoms are mechanical, you may find it helpful to read Move Well MD’s overview on nerve-related symptoms in their article on whether a chiropractor can help with a pinched nerve.
Technique is only half the story: daily habits that protect your spine
In NYC, neck and back pain often reflects daily load more than a single injury. The highest value changes are usually small and consistent.
For desk and laptop workers:
- Raise the screen closer to eye level and bring the keyboard/mouse closer
- Use short movement breaks (60 to 90 seconds) every 30 to 45 minutes
- Train mid-back mobility and scapular control if you live in forward-head posture
For people who lift, carry, or work in shipping, retail, or warehouses:
Stable surfaces and predictable loads matter. Even something as basic as using structurally sound pallets can reduce unexpected shifts while lifting and moving product. If your business sources liquidation or shipping platforms, choosing reliable suppliers (for example, bulk pallets for sale from established distributors) can be one small, practical way to reduce avoidable strain and sudden, awkward lifts that flare back pain.
Your clinician can also help you practice:
- Hip hinge mechanics (protects the low back during lifting)
- Bracing and breathing strategies
- Return-to-lifting progressions after a flare-up

What to expect from a chiro therapy plan for neck and back pain
While every case is different, a typical plan often moves through three phases.
Calm the flare-up
Early visits may focus on reducing pain and restoring tolerable movement. This is where manipulation or mobilization, soft-tissue work, and gentle mobility drills can be most helpful.
Restore function
Once pain is less reactive, the focus expands to strength, endurance, and movement confidence. This phase often includes rehab exercises and gradual exposure back to activities that triggered symptoms.
Maintain and prevent recurrence
Some people choose occasional maintenance visits, but the main goal is usually independence, meaning you have the mobility, strength, and strategies to manage minor flare-ups before they spiral.
If you’re comparing approaches, you may also want a deeper breakdown focused specifically on adjustments in the city, including technique options and who they’re best for. Move Well MD covers that in their guide on back adjustment in NYC.
Frequently Asked Questions
Is chiro therapy good for both neck pain and low back pain? Yes, chiro therapy is commonly used for mechanical neck and low back pain. The best approach depends on your symptoms, exam findings, and how irritable your pain is.
What’s the difference between an adjustment and mobilization? An adjustment (HVLA manipulation) is a quick, precise impulse. Mobilization uses slower, gentler movements through a joint’s range. Both aim to improve motion and reduce pain, but mobilization is often chosen when symptoms are more sensitive.
Does the “pop” mean the treatment worked? No. The popping sound is usually joint cavitation and can happen with or without benefit. Many effective techniques do not produce any sound.
How many sessions do you need for neck or back pain? It depends on the cause, how long you’ve had symptoms, your activity level, and whether you follow a rehab plan. Many people notice change within a few visits, but long-term prevention often requires exercise and habit changes.
Can chiro therapy help if pain shoots down the arm or leg? It can in some cases, but radiating symptoms should be evaluated carefully to determine whether a nerve root is involved and to rule out red flags. Your clinician may combine manual care with rehab, and sometimes refer for imaging or specialist care if needed.
Is it safe to get chiro therapy if you’re very sore or in spasm? Often yes, but the technique may need to be modified. In highly reactive flare-ups, clinicians may use gentler mobilization, soft-tissue care, and graded movement first.
Ready for a plan that fits your body and your lifestyle?
If neck or back pain is limiting your workday, workouts, or sleep, individualized care matters. Move Well MD is a Manhattan-based chiropractic and acupuncture clinic focused on helping patients move freely with an integrated approach that can include chiropractic care, acupuncture, physical therapy and rehabilitation, and comprehensive pain management.
To discuss which chiro therapy techniques make the most sense for your neck or back pain, you can learn more or request an appointment at Move Well MD.